MEDIAL KNEE PAIN FROM AN UNCOMMON SOURCE

Tid Bits of Info
- Pes Anserine or “goose foot” is a group of 3 tendons that insert in the proximal medial tibia.
- Abnormal biomechanics, primarily excessive valgus in the knee, can make someone more susceptible to developing PA symptoms.
- Two of the tendons of the PA, the gracilis and semitendinosus, are commonly used during ACL reconstruction surgery.
- Inserting an orthotic device in a shoe might stabilize the foot and eliminate excessive pronation.
- Seek the advice and treatment from a Physical Therapist if you suspect that you might have PA pathology.
Athletes and people from all walks of life experience sometimes experience medial knee pain (pain on the inside of the knee). While there are multiple reasons why a person may suffer medial knee pain, it is often misdiagnosed. The pes anserine (PA) helps to stabilize and move the knee joint and is placed under a tremendous amount of stress and strain during certain activities that can lead to an injury. Overlooking an injury in this structure leads to ineffective treatment.
The pes anserine is a structure that is made up of three tendons. They are conjoined and insert to the proximal, medial tibia. Their insertion takes on the appearance of a “goose foot” (pes anserine in Latin). The three tendons are the gracilis, sartorius and semitendinous. These tendons help to flex the knee and can be damaged during an activity that requires repetitive flexion of the knee joint. The tendons are “protected” against excessive rubbing on the medial tibia by fluid filled sac or bursa. This sac is wafer thin when healthy, but can become inflamed if the tendons apply too much force on it.
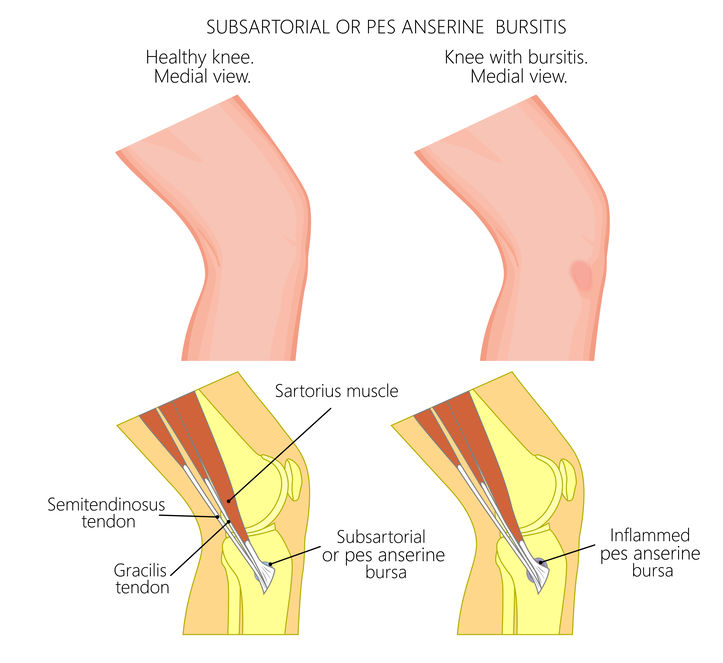
The PA supplies medial knee support and aides the static support structure, medial collateral ligament. These PA can be damaged if someone has excessive motion of the involved knee. One of the most prominent motions to cause excessive irritation to the PA is a valgus movement of the knee during gait. This valgus motion usually occurs due to the excess pronation of the foot and ankle during gait. This motion is commonly referred to as “knocked” knees and portions of the PA are stretched taut as the knee moves into the valgus position. When this occurs repetitively it can lead to excessive pressure on the bursa or damage to the tendon fibers. This is one reason why long distance runners are the most prone individuals to experience PA symptoms.
Injuries to the PA are usually in the form of tendinopathy conditions and/or irritation to the bursa causing bursitis. The diagnosis of these conditions can be tricky and distinguishing between the tendon pathology and bursitis is not always clear cut. The treatment of the condition is very similar and the combination of bursitis and tendon pain is the most frequently occurring condition.
The PA patient usually presents with pain and swelling in the medial proximal tibia. The involved knee might have limited motions in flexion and extension and the patient usually walks with a limp. The treatment consists of dealing with the acute symptoms and educating the patient on an exercise routine that will address the root cause (s) of their condition. In many instances, the weakness in the core and hip musculature can lead to abnormal biomechanics during gait.
Seek the advice and treatment from a Physical Therapist. These licensed professionals are skilled healthcare professionals that specialize in rehabilitation of musculoskeletal injuries. They are capable of evaluating and treating the PA symptoms. In the event that the symptoms do not resolve in a reasonable time period, diagnostic imaging might be required to fully assess the status of the PA.
The PA is a conjoined group of three tendons that help move and stabilize the medial aspect of the knee joint. If an individual performs an activity that engages the hamstring muscles excessively and they have abnormal biomechanics during gait, they are highly susceptible to developing PA symptoms. Treating the symptoms and correcting the abnormal mechanics must take place to restore normal function and reduce the chances of a reoccurrence.
























